How Insulin Resistance Can Cause Heart Disease
It’s a little known fact, but insulin resistance can cause heart disease and a lot of other unwanted chronic health conditions that will put a big crimp in your healthy aging plan. Here’s what to do about it.
Yes, it’s true — insulin resistance can cause heart disease.
If you’re scratching your head over that assertion — that insulin resistance causes heart disease, I can relate, because, perhaps like you, I would have said that the main culprit stems from some combination of too much saturated fat and cholesterol, and too little cardiovascular exercise. Although we’d be correct with that presumption, the typically-understood instigators of heart disease (fat/cholesterol/insufficient exercise) have a culpable partner: insulin sensitivity.
To know about and act on this insulin resistance/heart disease nexus will help ensure that as you get older, and the chances of a cardiovascular event gets greater, you will sidestep the masses.
The masses?
Yes, the masses. According to the CDC:
- Heart disease is the leading cause of death for men, women, and people of most racial and ethnic groups in the United States.
- One person dies every 36 seconds in the United States from cardiovascular disease.
- About 655,000 Americans die from heart disease each year—that’s 1 in every 4 deaths.
And according to the World Health Organization:
- Across Europe, cardiovascular diseases cause more than half of all deaths; and
- They are the number one cause of death globally.
I’ve written quite a bit about heart disease, typically focusing on preventative measures and what is usually thought of as the primary causes — LDL cholesterol and arterial plaque. But, as indicated in this post, there needs to be more focus on a major promoter of heart disease that doesn’t get enough attention — insulin resistance and it’s bedfellow, high blood sugar.
Thus, if you don’t want to end up like most everybody else (the “masses”), you need to make sure that your blood sugar is low, and your insulin sensitivity is high.
Insulin Resistance Can Cause Heart Disease
If your doctor hasn’t told you that insulin resistance can cause heart disease, he or she may not know about this connection. This is startling, because two-thirds of heart disease is not caused by fat or cholesterol, but by sugar and starch in our diet, causing insulin resistance. [1]
In fact, the central feature of almost all age related diseases — whether it’s heart disease, cancer, diabetes, dementia, sarcopenia (muscle loss), or hormonal imbalances — is insulin resistance.
So, what is insulin resistance?
Insulin resistance is a pathological condition in which cells fail to respond normally to the hormone insulin. [2]
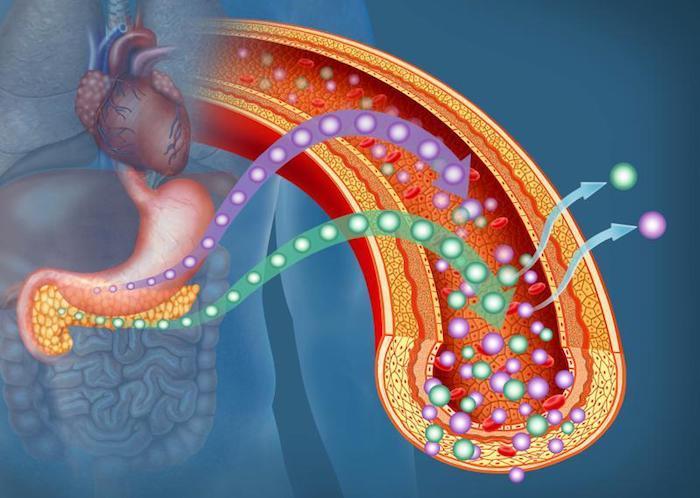
Insulin is a hormone that allows glucose to enter cells which also reduces blood glucose (blood sugar). Insulin is released by the pancreas in response to carbohydrates consumed in the diet. Insulin resistance occurs when excess glucose in the blood reduces the ability of the cells to absorb and use blood sugar for energy.
High insulin insensitivity has been associated with heart disease, stroke, many types of cancer, including breast, prostate, and lung cancer; and they’ve been associated with dementia.
Any of that can happen when we consistently consume boat loads of starch like flour, bread, pasta, rice, and refined grains and sugar. By “boatloads”, I mean the average American eats:
- About 152 pounds of sugar per person per year [3]
- A bit over 167 pounds of flour, per person per year (36 lbs corn, 131 lbs wheat) [4]
This makes up about 60% of our calories, makes us chronically ill and speeds up the aging process.
When diagnosed in middle age, diabetes reduces life expectancy by roughly 10 years. [5]
Worldwide, one person dies every ten seconds from diabetes-related causes.[6]
A Quick Primer On Diabetes
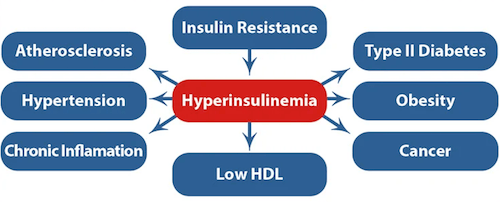
I encourage you to check out Life Extension Foundation’s Diabetes and Glucose Control health protocol. If you need incentive to do this, here’s a screenshot from their protocol indicating all the harm that can be caused from excessive blood insulin, which is called “hyperinsulinemia”.
Yes, too much insulin can mess up your health in many ways, especially by creating type 2 diabetes.
As Life Extension explains, diabetes mellitus is a condition characterized by high levels of glucose in the blood. Type 2 diabetes is far more common than type 1 diabetes (about 90% of diabetics are type 2) and is mainly caused by resistance to the effects of the hormone insulin, which facilitates removal of glucose from the blood. Type 1 diabetes is primarily caused by destruction of insulin-producing pancreatic beta cells.
Chronically elevated fasting blood glucose levels—or recurrent, excessive spikes in glucose levels after meals (referred to as postprandial) —can lead to devastating long-term consequences, such as heart disease, blindness, kidney failure, liver disease, and cancer. Abnormal glucose and insulin metabolism has been implicated in Alzheimer disease as well. In fact, this link is so compelling that many researchers have referred to Alzheimer disease as type 3 diabetes.
The Key To Healthy Aging Is Low Blood Sugar and Insulin Sensitivity
I remember hearing Dr. Mark Hyman say that one of the top cardiologists at Harvard told him that if you found a group of 100 year-olds with clean arteries, they would have one thing in common: they would be insulin sensitive.
This means that these individuals could perfectly regulate their blood sugar with very little insulin. This is one critical key to healthy aging. But there’s a problem, and that is only 12% of Americans are metabolically healthy, meaning they are not insulin sensitive like those 100 year olds with clean arteries. [7]
That 88% of Americans are metabolically unhealthy is disturbing, but unsurprising, given that 75% are overweight and between 20 and 40% of those who are of normal weight are nonetheless over-fat. You might have heard the description for that — “skinny-fat”. People with this profile are equally at risk of heart disease and aging, and all the other complications that we see happen to us as we age.
Whether you’re overweight and look it, or appear thin (in clothes at least), but are skinny-fat, the common denominator may be the consumption of too many simple carbs, meaning carbohydrates that are quickly absorbed, like sugar, and cause a fast spike in blood glucose (sugar). Too much of that and you can become insulin resistant.
After every meal you eat, your body’s blood sugar increases, and the body responds by producing insulin, the hormone that brings whatever you ate or drank into your cells so it can be used for energy. If you regularly eat complex, high fiber carbs, healthy fats and lean protein, your pancreas doesn’t need to produce much insulin and blood glucose doesn’t rise much.
But what can often happen as we get older, don’t take good care of ourselves, consume too many refined and processed foods, or live in toxic environments, we can develop insulin resistance. When that happens, the body becomes unresponsive to insulin, even if a lot is being made, resulting in weight gain, especially around the belly — the most dangerous place to carry fat. (Read Will Your Belly Fat Cause Cancer?
My Blood Sugar Story
As I show you in the screencast video below of my 23andMe genetic test, I may have a genetic propensity for adult-onset (type 2) diabetes. My father got it when he was my age, but his “lifestyle factors” worked against him; I’m beating that mine work for me.
I haven’t checked my blood sugar numbers for some time, but I have been on a routine cycle of taking a group of blood sugar control supplements, as well as eating mainly complex carbs and fibrous foods.
Without further adieu, the video:
Here’s the links I mentioned in the video:
- 23andMe genetic test
- 23andMe Genetic Data: Let Your DNA Optimize Your Health
- How Much Should You Weigh? Calculate Your Ideal Body Weight
What You Can Do About High insulin Resistance and High Blood Sugar
Here are five things you can do to address high insulin and blood sugar levels:
(1) Keep your insulin levels low
Try to get them lower than the “normal” range, because normal in a population of predominantly overweight people is not ideal. Excess insulin is clinically defined when levels are equal to or greater than 15 µIU/mL, which is the prediabetes/diabetes range. Life Extension believes an ideal insulin level to be <5 µIU/mL.
Check out Life Extension’s insulin test.
(2) Reduce belly fat
Before you work to reduce it, determine if your waistline is a problem.
Other than a mirror (or a friend who can duck a punch), there are two quick ways to assess if your belly is dangerously large:
- The waist-to-hip ratio, and
- The height-to-waist ratio.
For women, the waist-to-hip ratio should be no greater than 0.8, and for men, 0.9.
Use a cloth measuring tape, and measure halfway between the top of your hip bones, and the bottom of your rib cage (which for me is just over my belly button). Stand up straight, breathe in deeply, exhale, relax (don’t suck in your waist) and then see what the tape measure tells you. Then measure your hips at the place they’re most broad.
Divide waist number by hip number (Waist/Hips).
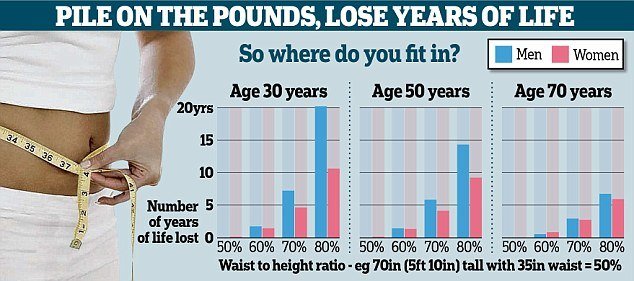
To measure your waist-to-height ratio, simply divide your height by your waist (waist/height).
As long as your weight-to-height ratio is half your height or less, you should live to the average life expectancy – which is currently around 81, says Dr. Margaret Ashwell, the lead scientist of a study about this measurement. But for every few inches over, you face losing months or even years of life.
(Read What Your Waist to Height Ratio Reveals About Your Health and How A Plant-based Diet Can Improve It.)
Congratulations if you don’t need to whittle away some belly fat. For the rest of the 99% of you, I’ve got your covered with these posts:
(3) Lower your high blood pressure
High blood pressure is a clue that you may have insulin resistance that’s beginning to cause heart disease. The Life Extension protocol on high blood pressure (hypertension) reports that studies support a target blood pressure for most people of 120/80 mm Hg, with an optimal level of 115/75 mm Hg. [8]
Life Extension cites a study that showed cardiovascular disease risk doubles for each increment of 20 mm Hg systolic and 10 mm Hg diastolic above 115/75 mm Hg. These findings become even more concerning when considering the staggering prevalence of higher-than-normal blood pressure: up to half of adults worldwide have blood pressure levels ranging from 120/80 to 139/89 mm Hg.
If your blood pressure is consistently above 115/75 mm Hg, check out their protocol to learn what you can do to help yourself. The typical stuff is covered, such as diet and exercise, but there’s also a few gems for you to polish, such as quercetin, a plant flavonoid shown to effectively lower blood pressure, and linked to lower cardiovascular risk.
Drinking celery juice and consuming two cups of blueberries (not all at once) five days a week is also helpful to lower blood pressure.
(4) Increase your low HDL
HDL stands for high-density lipoprotein, and it’s often referred to as the “good” cholesterol, as opposed to LDL (low-density lipoprotein), the so-called “bad” cholesterol. LDL delivers cholesterol to the cells that need it. HDL removes excess cholesterol from the bloodstream.
It can be problematic if your HDL is too low — under 50 mg/dL for women and 40 mg/dL for men. In either of these cases, there may be a problem with insulin resistance that can cause heart disease.
Here’s how to increase HDL:
- Consume about 4 tbsp (50 ml) of high polyphenol extra virgin olive oil every day for 6 weeks, [9].
- Do resistance training (weight lifting and calisthenics), particularly High Intensity Interval Training (HIIT). [10, 11, 12]
- Lose 1–3% of body weight. [13]
- Eat purplish plant foods, such as eggplant, red/purple cabbage, blueberries, blackberries and black raspberries. [14, 15]
- Take niacin, but be careful.
(5) Lower your high blood sugar
A fasting blood sugar level above 100 mg/dL can be a problem, and is far from the ideal mark of 85 mg/dL.
Yours is probably higher, but help is on the way. That’s because I’ve written several posts on how to reduce blood sugar. Read a few and you’ll be supercharged with what to do; of course, you will have to act on it.
Here’s the treasure trove, these among them:
Check out Life Extension’s glucose test.
Your Takeaway On How Insulin Resistance Can Cause Heart Disease
Remember these three things:
- Although the focus tends to be on excess LDL cholesterol as the main promoter of various forms of heart disease, insulin sensitivity, or lack thereof, needs to be reckoned with, because it has a major influence not only on cardiovascular health, but diabetes, obesity, systemic inflammation and more.
- You can determine if you may have an insulin, high blood sugar problem by getting the Life Extension tests for insulin and blood sugar, and to learn if your genetics influences this by taking the 23andMe test.
- You can help improve insulin sensitivity by (a) reducing belly fat (so that your hip-to-waist ratio is no greater than 0.8 for women, and 0.9 for men, or your waist-to-height ratio is half your height or less); (b) lowering your blood pressure (quercetin, blueberries, and this); (c) increasing your HDL through consuming high polyphenol extra virgin olive oil, resistance training and HIIT, losing body fat, eating purplish plant food and taking niacin.
Last Updated on February 7, 2024 by Joe Garma