Dr. Peter Attia – “How You Can Increase Healthspan”

Longevity expert Dr. Peter Attia shows you how you can increase healthspan, those years over which you’re healthy. Turns out, this is within your sphere of control.
DR. PETER ATTIA is a health speaker, researcher, nutrition and longevity expert, among other things. On November 25, 2017, BigSpeak Speakers Bureau published a presentation he gave about his “Reverse engineered approach to human longevity” on Youtube.
If you have a spare one hour and 15 minutes, I urge you to watch it (below). If you’re not familiar with the science of longevity or need a faster way to get what Dr. Attia has to say, scroll down and read my summary of this presentation.
Here’s what you’re going to learn:
- The four components of healthspan and the Longevity Curve;
- What we learn from centenarians and their genetics;
- The three anti-aging pillars — caloric/dietary restriction, rapamycin and the molecular insights of nutrient sensing, autophagy, senescence and inflammation; and
- Healthspan tactics — what you can do.
Let’s dig in…
The Focus: Increase Healthspan
Let’s begin with a simple graph. It’s instructive to do so because it ably shows the difference between “healthspan” and “lifespan”, the two components of longevity. lifespan ends when you die, but healthspan is variable, given that it’s a qualitative measure, not one tied to the inexorable march of time.
Dr. Peter Attia thinks of healthspan as having four parts:
- Mind (cognition);
- Body (physical capacity);
- Freedom from pain; and
- Stress tolerance.
Mind
You can think of your mind as that thing that produces cognition. Parts of it can be objectively measured, such as short-term memory, executive function, processing speed and stress tolerance.
If we have the misfortune of experiencing neurodegenerative disease as we get older, it’s short-term memory that first slips away. That can be irritating, as is the decline of your ability to do a calculation or look at data and quickly make an inference — all of which tends to slow over time — but all this pales in comparison to what most people hold dear, executive function.
When executive function substantially declines in the later stages of dementia, death can be close at hand.
Physical capacity
The second part of healthspan is the body, or physical capacity. The issue here isn’t necessarily physical performance, such as how many seconds you can sprint 100 meters, or how many pull-ups yo can do, but rather has to do with:
- Muscle maintenance, important for both structural and biochemical reasons
- Functional movement, such as having flexibility in your spine and being able to do a hip hinge (the lack of which is responsible for 80% of the physical morbidity that he observes, as well as a few common muscle imbalances, says Dr. Attia; morbidity referring to the quality of being unhealthy).
Freedom from pain
If you’re in chronic pain, not much of anything else in life matters. Unfortunately, as we age, pain happens, as the discomfort of our chronic injuries and diseases multiplies.
Stress tolerance
This is a set of tools at your disposal to cope with physical or emotional pain that is either chronic or acute. Consider a person’s emotional stress and corresponding reaction to being stuck in traffic. For some people, inching along in traffic is stressful; for others, not so much.
People have vastly different capacities to cope with distress. Those with little stress tolerance can easily be aggravated, while others who have a buffer of distress tolerance are not stressed by the same things.
Sense of purpose and social support
There’s clearly a positive relationship between long-term health and a person’s sense of life purpose and his/her connection with others, be it family, religion or social causes.
It’s very difficult for someone to have a great quality life, Dr. Attia observes, if they are not doing well on these four metrics, which are not absolute, but a useful way to think about important factors that can increase healthspan.
Which leads me to the Longevity Curve. This is how the longevity cure looks like for the average person in U.S:
Dr. Peter Attia’s Longevity Curve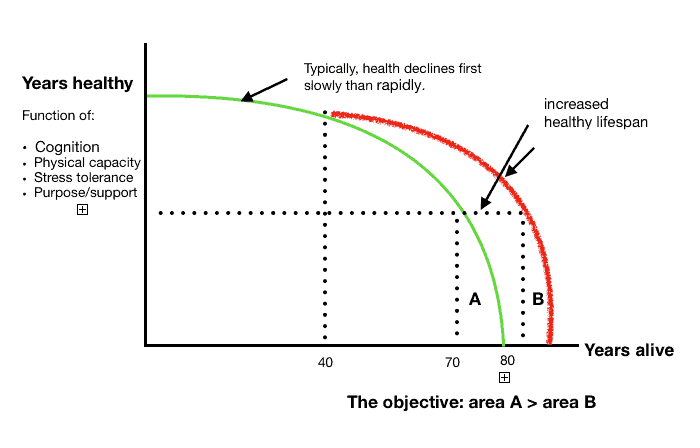 The aim is to fix three things of Longevity curve:
The aim is to fix three things of Longevity curve:
- Increase the number of years we’re alive (red line)
- Delay the rate of decline (red line)
- Compress the period of morbidity (area “B” is less than “A”)
Lessons of the Centenarians
There are two fundamental takeaways we can glean from centenarians, says Dr. Attia.
(1) Their experience of chronic disease is delayed
Of those who die over the age of 40,who don’t smoke or are suicidal, 80% will die from the four horsemen of death:
- Cardiovascular/cerebrovascular disease
- Cancer
- Neurodegnerative disease (like Alzheimer’s)
- Accidental death (automotive, accidental poisoning and falling)
How about centenarians — how do they die?
Pretty much the same as the rest of us, with these slight differences:
- Higher percent from cardiovascular/cerebrovascular disease;
- Lower percent from cancer;
- About same for neurodegenerative disease; and
- More pneumonia.
So, it’s not that centenarians are immune to dying, it’s just that they get the chronic diseases that typically kill us all later than non-centenarians. Centenarians commonly do not acquire their first clinical sign of these diseases until they are between 80 and 98 years old. The rest of us get the early clinical manifestations of these diseases about twenty years sooner, which leads us to the most valuable insight centenarians offer:
The key to living longer is delaying the onset of chronic disease.
Yes, pretty obvious, but it’s worth underscoring because disease compounds, meaning disease digs into us well before we succumb to it. Hence, the question is what could be done to slow the rate of progression of chronic disease, because that’s the ticket to living longer and healthier.
(2) Their longevity is highly influenced by their genes
Centenarians in the U.S. represent 0.4% of the population. Interestingly, the average centenarian is no more likely to do or engage in healthy behavior than non centenarians; in fact a number of studies have shown that some are more likely to smoke and less likely to exercise.
Given this, the basic premise is that centenarians have longevity in their genes, which is correct, but if you dig deeper, the revelation is that they’re more similar to the rest of us than you’d think at first blush.
There are about a dozen or so genes that tend to cluster in people who live longer. A few examples of common genetic differences we see an exceptionally long-lived people are that they tend to have:
- Hypoactive C3
- Hypoactive PCS K9
- ApoE2 > ApoE3 or ApoE4
- Less GHR
- Less IGF-1
Let’s unpack this terminology and what it all means.
“Hypo” means less (the converse of “hyper”), so “Hypoactive” is less active than some standardized norm.
The value of understanding the phenotype of those among us who live healthier, longer is to check what we can do to acquire their phenotype. Of course, we can’t reverse engineer our genetics, but we can do things that can affect our physical characteristics (phenotype) to mimic theirs.
Hypoactive (low) C3
Hypoactive CA is characterized by lower triglycerides and lower ApoB, which is among the most important biometrics to understand cardiovascular risk because these are proteins found in lipoprotein particles that are artery-clogging.
Hypoactive (low) PCS K9
If you have hypoactive PCS K9, there is much more LDL (the “bad” cholesterol) receptors on your liver. They then clear ApoB bearing particles out of blood circulation with an alarming degree of precision. That’s good.
ApoE2 > ApoE3 or ApoE4
Less GHR
GHR is “Growth Hormone Receptor” and the reason you want less of it is because its deficiency is associated with a major reduction in pro-aging signaling, cancer and diabetes.
Less IGF-1
IGF-1 (“insulin growth factor-1”) is a hormone similar in molecular structure to insulin. The evidence suggests a slight increased risk of some cancers due to higher activity of the IGF system. Conversely, patients with congenital deficiencies in IGF-1 have a protective effect against developing cancer.
Thus, those that have these genes are more protected from the chronic diseases of the Four Horsemen. Those who do not need to learn lifestyle behaviors that can mimic them.
Three Anti-aging Pillars
If you weren’t born with the genes of a centenarian, what do you do? You can’t scurry about and find some, but you could learn about the three things that seem to increase healthspan, maybe even lifespan, and try them out.
These three things, or Pillars, have worked across several animal species (from worms to monkeys) and are presumed to be applicable to humans as well.
I. Caloric Restriction vs Dietary Restriction
What’s been clearly shown in experiments on yeast, worms, fruit flies, rodents and monkeys is that reducing calories (CR) and dietary quality (DR) improves healthspan and lifespan.
In the case of CR, the number is about 30% below what the metabolic rate and activity level dictates. In the case of DR, the formula of which specific nutrients are best wasn’t clearly established when Dr. Attia gave this presentation in 2017. Since then, however, Dr. Valter Longo’s studies on fasting mimicking diets have been released, leading to his ProLon Fasting Mimicking Diet, which basically combines CR with specific DR nutrients in a 5-day program intended to be done two or more times a year.
Read The Prolon Fasting Mimicking Diet
How it became clear that DR played a key role in the effectiveness of CR was by comparing two famous CR monkey experiments, one done at the University of Wisconsin and the other at NIH (National Institutes of Health).
There was a lot of confusion in 2009 when these two studies were first compared, because it appeared that in the Wisconsin study, CR did as hypothesized (the monkeys who ate less had a survival advantage over those who did not); whereas in the NIH study there was no difference between CR and those monkeys that ate when and as much as they wanted (ad libitum).
This confusion got cleared up when the diets given to monkeys in the respective studies were examined.
NIH monkeys were consuming a diet that somewhat resembled their normal diet, which was very low in sucrose. The Wisconsin monkey experiment used a liquid formula to feed the monkeys that tasted so awful that it was spiked with sucrose, resulting in a formula that was 25% sucrose; shockingly sweet.
Given the outcomes of the Wisconsin and NIH monkey CR studies, Dr. Attia and others surmise the following:
- The NIH CR monkeys didn’t live longer or healthier than those who fed ad libitum because they both ate healthily (DR), and therefore there wasn’t a significant benefit from eating less (CR).
- The Wisconsin CR monkeys did live longer and healthier than those who fed ad libitum because they ate less of a high-sucrose diet and given how unhealthy that was, eating less of it enabled better outcomes for that group.
So how do you mimic CR; meaning, how to get the benefits of under-eating every day without the misery of doing so?
You can mimic it by intermittently fasting on a daily basis, or you could intermittently fast on a monthly basis or something similar, such as Dr. Longo’s fasting mimicking protocol.
II. Rapamycin and Genetic Insights
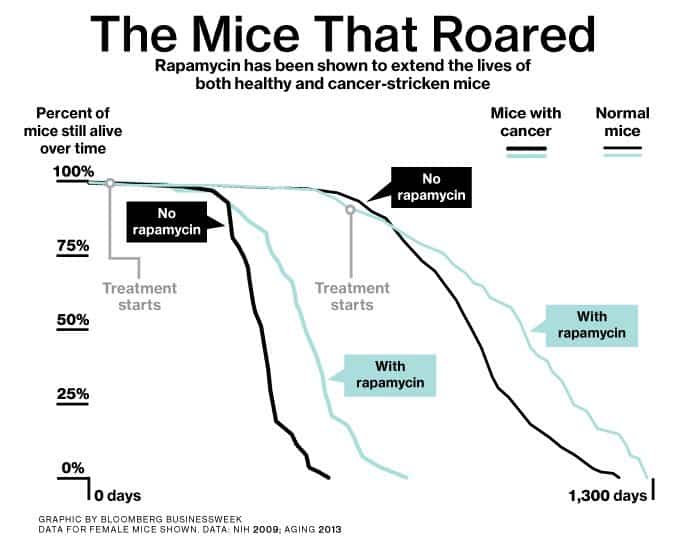
Rapamycin extends life across the animal spectrum upon which it was tested.
This is related to CR/DR because Rapamycin works through mTOR, and they both are involved in something called “nutrient sensing“.
Anti-aging and science author Bill Gifford describes mTor:
“MTOR is like the circuit breaker in a factory: When it’s activated, the cell grows and divides, consuming nutrients and producing proteins. When mTOR is turned down, the “factory” switches into more of a conservation mode, as the cell cleans house and recycles old proteins via a process called autophagy.”
Dr. Attia wisely sidesteps going deeper into this area given it’s complexity, but in my article, Do These 2 Anti-aging Pills Really Work, I urge readers not to try to experiment with Rapaymin yet even though it sure seems good for mice:
Scientists do genetic testing on organisms. When they find similarities across a broad spectrum of organisms, say from yeast through monkeys, there’s a tendency to think such findings might also pertain to humans.
The longevity benefits of Rapamycin have been proven in many organisms, and last I heard there’s an ongoing study to see if it will improve the lifespans of dogs.
Then there’s IGF-1 to consider.
The DAF-2 gene encodes for the insulin-like growth factor 1 (IGF-1) receptor in the worm C. elegans, which has a remarkably similar longevity curve as humans. This worm lives 18 days; half of that time in robust form, the other half in decline.
Turns out that if you shut off the DAF-2 gene a bit, the worm doesn’t survive, but if you attenuate it a bit, it can live two and one-half times longer! And there’s almost no period of decline. One day doing great, the next day in worm heaven.
This is the mortality curves of a non-manipulated regular C. elegan and those with DAF-2 gene manipulation:
That square “curve” represents the worms with DAF-2 gene tweaking. They live over twice as long and then rather than experience a slow decline, boom — fast death.
So, what do these worms have to do with you?
Turns out, the Daf-2 gene codes for a receptor that in the worm does something very similar to what our insulin and IGF-1 receptors do in us, which begs the question: Is this a genetic insight for us, one that could work for our longevity and health as well?
Scientist who study such things tend to think that the many genetic insights gleaned from the various organisms studied can be applied, perhaps with some changes, to us.
III. The molecular insights
From the understanding gleaned from experiments with CR, DR, Rapamycin (and Metformin, I might add) comes a whole series of insights, perhaps the most important being the respective roles of:
- Nutrient sensing;
- Autophagy;
- Senescence; and
- Inflammation.
Let’s touch on each of these.
Nutrient Sensing (fewer, better)
These days we’re flooded with food. Think about it — how often are you more than ten steps away from being able to grab and gobble down some food?
Dr. Attia points out that we didn’t evolve in the food-abundant environment in which we currently live. Humans have been exposed to the nutrient abundance existing today for an infinitesimally tiny fraction of our genetic existence, and thus we are not optimized to be eating so much so often.
It makes sense, then, that withdrawing from food (CR) and/or limiting/optimizing nutritional intake (NR) would have a positive impact on our health, if not our lifespan.
Which brings us to Autophagy.
Autophagy (less is more)
As I wrote in How Intermittent Fasting Ignites Cellular Autophagy and A Longer, Healthier Life, the 2016 Nobel Prize in Medicine was awarded to Dr. Yoshinori Ohsumi for his discoveries on how cells recycle their content, a process known as autophagy, a Greek term for “self-eating.”
Here’s how I put it:
“Cellular autophagy is a crucial process for cells to survive and stay healthy, says the New York Times, which translates to your survival and health. During a period of ingesting limited calories, or starvation, not only do cells break down proteins and nonessential components and reuse them for energy, but also cells use autophagy to:
- Destroy invading viruses and bacteria; and
- Rid themselves of damaged structures; a process which…
- Is thought to get disrupted in cancer, infectious diseases, immunological diseases and neurodegenerative disorders; including Parkinson’s disease, type 2 diabetes and cancer.” (More here.)
Dr. Attia mentions that there’s probably an overlap (or relationship) between Nutrient Sensing and Autophagy, but doesn’t elaborate. Curious, I did some pecking around to see if I could uncover what he might have referred to. Sure enough, there’s an abundance of literature that delves into the connection between the two.
Nature.com gets the ball rolling with this:
“Nutrient signalling encompasses various cell signalling pathways that are regulated by nutrient availability. Changing nutrient levels activates signalling cascades that modulate fundamental cellular processes including metabolism, proliferation, secretion and autophagy.” (source)
And the study, Autophagy regulation by nutrient signaling connects the dots thus:
“One of the key cellular responses to nutrient withdrawal is the upregulation [increase] of autophagy. Recently, there has been a rapid expansion in our knowledge of the molecular mechanisms involved in the regulation of mammalian autophagy induction in response to depletion of key nutrients.”
To sum it up:
Less food, more cellular house cleaning, more health.
Senescence (the zombies)
Simply put, cellular senescence is a phenomenon by which normal cells cease to divide; meaning, they no longer proliferate.
That’s good during much of life when the body needs to heal wounds and suppress tumors (and cancer), but as we age there tends to be a steady accumulation of senescent cells that has adverse consequences. The problem with too many senescent cells is that they’re pro-inflammatory, and can, in effect, poison healthy cells and thereby contribute to aging-related diseases and morbidity.
In animals models, when “you knock these cells out, you reverse the aged phenotype”, says Dr. Attia.
Read Can 4 Natural Compounds “Eliminate Senescent Cells” and Prolong Your Healthy Lifespan?
Inflammation (a ubiquitous part of aging)
If there was no such thing as inflammation, you couldn’t heal from a cut on your hand. When inflammation is mobilized to heal a specific thing, it’s generally good. When it’s systemic — happening all the time, everywhere — it’s bad.
Dr. Attia points out that it’s important to underscore the role that inflammation has in cerebrovascular/ cardiovascular disease, because these diseases kill the most people.
Read 14 Ways to Wipe Out Chronic Inflammation (and why you need to)
So, now you have a sense of these “pillars”, let’s get more explicit about how they can be applied to your life.
Tactics to Increase Healthspan — what you can do
These are the four most important things you can do to increase your healthspan that is within your scope of influence, according to Dr. Attia:
- Nutritional Biochemistry;
- Exercise Physiology;
- Sleep Physiology; and
- Distress Tolerance.
Let’s touch on each.
Nutritional Biochemistry
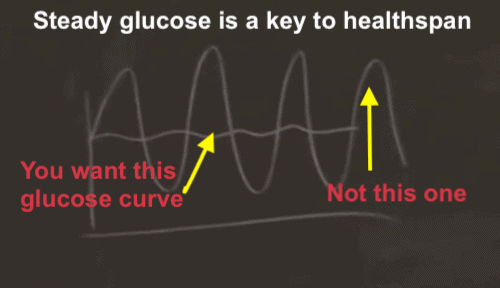
Dr. Attia’s best nutritional advice is to mange your carbohydrate consumption such that your blood sugar can be maintained at 85 mg/dL or lower.
This is empirically verifiable, he says, which shows that an average daily blood sugar reading of 85 mg/dL — with a modest 15 mg/dL variation up or down — will lead to low insulin AUC (which refers to “Area Under Curve”, a measure of insulin sensitivity.)
As long as the focus is on low, steady blood glucose (sugar), Dr. Attia is diet-neutral. Paleo, vegan, keto — have at it, just keep up an average of 85 mg/dL with low variability (none of those big spikes in that graph above).
With protein the approach is going to be a barely positive nitrogen balance. Excess amino acids — beyond what is needed to maintain your lean muscle tissue — may lead to problems. Amino acids, the “the building blocks of proteins“, play a very important role in nutrient sensing pathways, and a number have been implicated in disease progression. (He’s referring to excess protein.)
The key is to consume the protein you actually use to support your lean body tissue (like muscle). there’s a fine balance between how much protein you need to maintain muscle mass versus what is too much where it starts to become harmful.
Regarding fat intake, Dr. Attia’s belief is that at a caloric level it ends up being the balance after protein and carbs are adjusted for your requirements.
He’s deliberately vague on this score, because:
“I can’t just give you a prescription. I can’t say eat this many grams of carbohydrates. What I can say is you eat as many grams of carbohydrates as you can tolerate to do this (glucose homeostasis), and for some people that’s a lot of carbohydrates and for some people it’s not a lot of carbohydrates. And so carbs and protein are highly dependent on the individual, on how much they exercise as I’ll explain in a moment how well they sleep how well they manage to stress —all of these things feed into this. … it effectively becomes a function of fuel partition — how well you partition fuel, which is dependent on certain genetic factors like how much lipoprotein lipase you express on muscle cells versus fat cells, and also a number of things that are related to these other interventions.”
Fat, then, effectively becomes the balanced calorically by how many more calories you need after accounting for protein and fat calories, given your basal metabolic rate plus your activity level.
If this sounds confusing it’s because it is. Dr. Attia simply can’t tell you what combination of macronutrients (carbs, protein and fat) is ideal for you. And without testing it, no one can.
Exercise Physiology (build a big glucose sink)
When it comes to exercising with the aim of increasing healthspan/lifespan, you can put performance aside and ask what’s the necessary dose of exercise to experience a long and strong life.
Through this lens, the focus needs to be on the metabolic advantage of exercise. Here, again, it’s about glucose.
The body can put glucose away quickly into only two places, the liver and the muscle. The liver has a relatively finite capacity for glycogen. Muscle has a much more elastic capacity for glycogen, which means, the larger the muscle the more insulin sensitive the muscle, and therefore, the more glucose that it can dispose.
For healthspan/longevity purposes then, the goal is to have muscles that are really big sinks for glucose. The bigger your sink is and the more efficiently it can take in glucose with a lower level of insulin is a marker for insulin efficiency/sensitivity. And, thereby, the more carbs you can tolerate.
This has been proven. Dr. Attia recounts a study he reviewed that took muscle biopsies from people who were pre-diabetic. It showed that the single greatest predictor of type 2 diabetes was insulin resistance in the muscles.
If you don’t like exercise, just one type, says Dr. Attia, and that’s strength training:
“I tend to divide this into two categories. If you enjoy heavy hip hinge compound joint movements like dead lifts and squats, great — you learn to do those correctly and they will serve you indefinitely in life and that includes if you’re 90 years old.”
If the idea of lifting something heavy off the floor makes you want puke, know that you can benefit a lot from a “super slow” weightlifting protocol. In this case, because you’re moving the weight so slowly, it can not be accelerated and thereby can’t be very heavy. Also, again, because you’re moving the resistance slowly, there’s more “time under tension” than is true with conventional weight lifting.
The net effect of super slow lifting is that, like big, heavy compound movements like squats and dead lifts, slow lifting activates the type II-b muscle fibers activated, which is rarely experienced unless you pretty much exhaust the muscle.
In Dr. Attia’s case, his exercise consists of weight lifting and interval training, which is either done on a bike, on a stationary bike or on a treadmill.
Workout hard, get younger and sleep like a baby.
Sleep Physiology
Sleep quality is widely underappreciated. There’s this mentality promoted by some high achievers that “I’ll sleep when I’m dead”, which will come sooner than later if sleep isn’t given its due.
Sleep is among the most highly conserved behaviors of our species that doesn’t seem to go away (meaning, it’s been with us since we were us). Humans have typically always spent about one-third of their lives sleeping. There must be a good reason for it.
Dr. Attia tells the story of how his sleep-deprived medical residency knocked down his testosterone. It was so low that once he began sleeping for eight hours again, his testosterone elevated nearly seven-fold! He attributes this to the “certain things the brain is able to do during slow-wave sleep”.
Sleep is divided into alpha wave, delta wave, theta wave and a couple of these spindles that show up on EEG, but in particular the delta wave or slow wave sleep seems to be where our pituitary gland actually puts out Follicle-stimulating hormone (“FSH”, a regulator of the development, growth, pubertal maturation, and reproductive processes of the body) and Luteinizing hormone (“LH” a hormone that supports our reproductive system.)
When you get enough sleep, your body is not only better at making testosterone and the other sex hormones, but your memory gets better too. The hippocampus controls the consolidation of memory and is sensitive to sleep disturbances, so if sleep is disrupted, so is your memory.
Also your blood sugar.
Yes, blood sugar once again!
Dr. Attia relates a University of Chicago experiment that measures the effect of four hours of sleep on glucose by using something called “Glucose Clamps”.
The glucose clamp technique is a method for quantifying insulin secretion and resistance. It is used to measure either how well an individual metabolizes glucose or how sensitive an individual is to insulin.
The glycemic clamps of the Chicago experiment subjects deteriorated by 50%; meaning, they were much less able to clear glucose from their blood.
Distress Tolerance
Dr. Attia had to skip distress tolerance because he was running out of time, so I’ll take a crack at it.
The first thing I want to convey about managing stress is if you don’t, you might just die quicker, that is if Nobel Laureate Dr. Elizabeth Blackburn is right that shorter telomeres lead to a shorter lifespan. If you need to learn how to handle chronic stress better, read my article, How Depression and Stress Make Us Age Faster.
I don’t mean to be glib, but the fastest, best way to reduced stress/depression is to go get a hug. Hugging someone you care about makes your brain produce dopamine. Dopamine is the “love hormone” and, as you might expect, makes you feel better.
Another thing you can do when stressed is practice the military’s 4x4x4 breathing technique. If they can become calm when mortars are landing nearby, just think of what you can do in traffic. More on that here.
Your Takeaway
There’s a lot to unpack, but it’s pretty straightforward if we stay away from the science.
Remember that to increase healthspan and possibly your lifespan distills down to these seven things:
- Eat less on a regular basis, say a few consequent days in a month, or every few days or most days by eating during a constrained feeding window, say 1:00 pm till 8:00 pm.
- Eat highly nutritious foods, which pretty much means no sweet drinks, fast food, processed food, sugar or “simple” carbs (pasta, potato, white bread, white rice, etc.)
- Know your blood sugar number and attempt to get it down to 85 mg/dL. Tips here.
- Grow muscle. This has nothing to do with getting “muscle bound” and everything to do with improving your body composition by having more of it consist of muscle, less of it fat.
- Reduce inflammation. Check out how the right curcumin supplement and Dr. Weil’s anti-inflammatory diet could help.
- Reduce stress by first learning to acknowledge when you’re stressed (be mindful), then applying a technique to work your way through it.
- Get some deep sleep, seven to nine hours of it. It’s helpful if you turn off all blue light (screens) and hour before bed time, soak in a tub, sip hot herbal tea and make sure that your bedroom is very dark. (I do that by wearing a sleep mask.)
Before you go, check out Dr. Peter Attia’s “Top 5 Biological Tests Everyone Should Take“.
Last Updated on September 29, 2022 by Joe Garma