How To Fix Your Adrenals and Rev Up Your Life
In this day and age of hustle bustle, everyone seems stressed out. And maybe we are. There’s a pretty good chance you need to fix your adrenals. Find out if you’re at risk for adrenal fatigue and what to do about it.
(Scroll down for the video.)
HORMONES ARE exceptionally important and complicated chemical messengers that control or influence most of our major bodily functions, from simple basic needs like hunger to complex systems like reproduction, and even emotions and mood.
It’s simply not possible to maintain a youthful vitality and healthy life if your hormones are not balanced and in harmony.
This past week, I was writing the hormone chapter in my forthcoming book and wanted to begin it by addressing the most prevalent and significant hormonal dysfunction experienced by most of us. I was surprised to learn that the hormonal dysfunction that fits that description is adrenal fatigue.
Simply put, adrenal fatigue is caused primarily by chronic stress and poor lifestyle choices, both quite evident in the hectic lives many of us experience nearly every day.
Adrenal expert Dr. Michael Lam says that over 50% of the U.S. population experiences adrenal fatigue. Dr. Josh Axe puts the number at 80%. There’s a good chance, therefore, that you need to fix your adrenals, or you know someone who does. Things can get bleak if you don’t.
For instance, adrenal fatigue:
- Dramatically reduces a person’s ability to tolerate stress, both emotionally and physically;
- Can experience depression and listlessness; and
- Can trigger hypothyroidism and insulin resistance.
A man might think that the most important hormone for him is testosterone, and a woman might give the nod to estrogen. These are sex hormones that represent reproduction, a very important drive, but not as important as survival itself.
The body will convert the sex hormones into adrenal hormones to maintain survival at any cost, which is why when you’re stressed and tired, your sex drive goes down. There’s no point, then, in getting all flummoxed about the sex hormones (progesterone, testosterone, and estrogen) before you evaluate the health of your adrenals.
Survival is always more important that reproduction, and the body will do what’s needed to survive. The adrenal glands and their hormones represent survival – this is about the “fight or flight” mechanisms required for us to escape mortal threats and live another day
You need to know about the importance of your adrenal hormones simply because they’re critically important to your health, and yours may be compromised to some degree.
In this article, you’ll discover:
- What are the adrenals;
- Why the relationship between DHEA and cortisol is critical;
- How we respond to stress is largely up to us;
- Useful suggestions for lifestyle changes, nutrition and supplementation; and
- The best ways to test your adrenals.
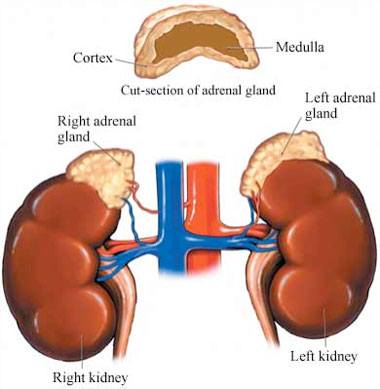
Let’s begin with a picture of the adrenals:
Your adrenal glands are triangular in shape, located above your kidneys and act as your body’s energy reservoir. They’re integral to your capacity to handle stressful situations, for proper functioning of your immune system, proper production of white blood cells, and muscle strength and tone.
The adrenals come in two parts, the inner region, which is known as the adrenal medulla, and the outer region, which is called the adrenal cortex.
The adrenal medulla is responsible for producing and regulating a class of stress hormones known as catecholamines, which include adrenaline, noradrenaline, and dopamine. Catecholamines help your body respond to emotional upheavals, stress, low blood pressure, low blood sugar levels, exposure to extreme temperatures, lack of oxygen, and danger, all of which can activate the “fight or flight” response.
The hormones produced by the adrenal cortex are known as steroidal hormones. There are three classes of steroidal hormones:
- Mineralcorticoids, which help regulate your body’s fluid balance via regulation of the kidneys as they interact with sodium and potassium;
- Glucocorticoids, which help metabolize carbohydrates, proteins, fats, and sugars, as well as helping to maintain proper blood pressure levels; and
- The sex hormones (androgens and estrogens), which oversee the health of your sex organs.
In its capacity to control the body’s response to stress, the adrenal glands produce adrenaline, which gives us the instant juice to react to a stressful situation by fleeing from it (“flight”) or confronting it (“fight”).
The adrenal glands also produce cortisol and DHEA, which enable the short or long term stress hormone responses, and must be in balance with each other, which I’ll address below.
In his book, Outstanding Health: The 6 Essential Keys To Maximize Your Energy and Wellbeing, hormone expert Dr. Michael Galitzer writes that adrenal fatigue (or “burnout”) is among the most common health conditions experienced by his patients. And yet it’s typically not diagnosed by most doctors.
Dr. Galizer points out that adrenal failure is identified by traditional medical practitioners as Addison’s disease, a condition that President John F. Kennedy had, but that the most prevalent issue experienced isn’t adrenal failure, but adrenal fatigue (when the adrenals are depleted), which is largely being ignored.
On page 277 in his book, Dr. Galizer writes:
Physicians don’t look for it. They don’t properly diagnose it, and they don’t treat it correctly. When patients come to me and complain about lethargy, fatigue, lack of energy or a reduced sex drive, or that they just don’t have the same energy or the same sex drive, in almost all cases at the root of their problems, especially if they are past their thirties, can be traced back to impaired adrenal gland function. So working to restore and optimize their adrenal function is usually where I start.
I mentioned above that there’s no point in first trying to balance your sex hormones if your adrenals are compromised because survival trumps reproduction. If you’re experiencing adrenal fatigue, your body will convert the sex hormones into adrenal hormones to maintain survival at any cost.
Therefore, you’ve got to maximize adrenal function first. The adrenal system is the key system to your overall health, and ignoring it is perilous to your health.
Take a pregnant woman for example.
As Dr. Galizer explains it, if a woman is chronically stressed when pregnant, she will start converting her own progesterone – now at a higher level during pregnancy than normal — into the adrenal hormones.
At the seventh month of pregnancy, her baby’s adrenals begin to function. If at this point the mother’s adrenal glands are compromised, her body will use her baby’s adrenals to support her own. In turn, this parasitic-like action makes the baby’s adrenal glands work harder to supply excess adrenal hormones required to both itself and the mother.
Once the umbilical cord is cut at birth and the mother is unable to continue relying on the baby’s supply of adrenal hormones, she may experience postpartum depression and fatigue. Moreover, in this situation the newborn may become hyperactive, develop colic or other health problems, all as a result of how his or her developing adrenal gland system was affected by the mother’s stress while the baby was in the womb.
The DHEA and Cortisol Dance
When adrenal fatigue or burnout occurs, the adrenal hormones that require the most attention are cortisol and DHEA.
As adrenal-produced hormones, cortisol and DHEA act as antagonists that need to be maintained in a certain ratio, although what that ratio is seems illusory. Suffice to say that cortisol and DHEA do a balancing act, or dance, and it must be fluid for one not to, in effect, trip over the other and come crashing down.
Cortisol and DHEA are steroid hormones, both synthesized from pregnenelone, the master steroid hormone, which is derived from cholesterol. In many ways, the Cortisol to DHEA ratio modulates biological energy output, and their effects are felt at the cellular level all over the body.
Cortisol
Cortisol is a life sustaining adrenal hormone essential to the maintenance of homeostasis. (As concerns physiological processes, homeostasis is the tendency toward a relatively stable equilibrium between interdependent elements.)
Cortisol is called “the stress hormone,” because it influences, regulates or modulates many of the changes that occur in the body in response to stress including, but not limited to:
- Blood sugar (glucose) levels.
- Fat, protein and carbohydrate metabolism to maintain blood glucose (gluconeogenesis).
- Immune responses.
- Anti-inflammatory actions.
- Blood pressure.
- Heart and blood vessel tone and contraction.
- Central nervous system activation.
Whereas too little cortisol causes the life threatening Addison’s disease that President Kennedy suffered from, too much cortisol suppresses the immune system, breaks down tissues and has a catabolic effect that in extreme cases can lead to Cushing’s syndrome.
DHEA
DHEA (dehydroepiandrosterone) is called an androgenic hormone. It‘s a precursor for testosterone and the estrogens.
DHEA is a very powerful anti-aging hormone. Low levels of DHEA are found among those with Cancer, CVD, Alzheimer’s, Diabetes, Depression, Hypothyroidism and Adrenal Fatigue.
DHEA also antagonizes the catabolic effects of cortisol. What this means is that DHEA acts to rein in excess levels of cortisol that, if persistent, can tear down body tissues (catabolism, not to be confused with “cannibalism”.)
As mentioned, since cortisol and DHEA have opposing effects, they should be viewed together as a ratio, given that they work together through their alternating, dualistic balance, says nutritionist Michael McEnvoy in his article, Cortisol & DHEA: The Major Hormone Balance.
When cortisol is elevated disproportionately to DHEA, the ratio is higher, and in this situation numerous biological effects are augmented.
Here are some of the major effects of the Cortisol to DHEA ratio:
- The balance of pro/anti-inflammatory stasis.
- Immune Regulation. Remember that cortisol suppresses immune function.
- Protein, Fat and Glucose metabolism. Evidence suggests that hyperglycemia, which can result in diabetes, in many cases can be caused specifically from imbalanced cortisol and DHEA levels.
- Thyroid, Pancreas and ovarian function.
- Detoxification capacity. Since the body needs energy to properly deal with toxic metals, the hormones produced by the adrenal glands are considered to be the cornerstone to heavy metal and xenobiotic elimination.
- Skeletal health. High levels of cortisol can cause breakdown of bone as well as the collagen matrix that holds bone together.
- Memory. DHEA is a critical component for brain function and cognition.
- Cortisol and DHEA have intrinsic relationships with numerous other steroidal hormones such as progesterone and aldosterone. If adrenal function is compromised, the body may bypass the pregnenelone to progesterone to cortisol pathway and “steal” pregnenelone. This can cause numerous complications including the transference of progesterone into androgenic testosterone.
The Stress Response
Let’s look at a typical situation.
When you wake up, your cortisol levels are naturally elevated so that you’ve got some “get up and go”. As you can see in the chart below, cortisol levels begin high in the morning, drop precipitously thereafter, and rising only in response to food.
The natural rhythm of cortisol production depicted in the graph above is disrupted when you’re stressed. When you’re stressed cortisol levels go up, and if that high level is sustained, you may have a hard time sleeping given that your cortisol level will be high in the evening when it should be low. This, in turn, interferes with your body’s ability to produce melatonin and growth hormone, both of which promote healthy, restorative sleep.
When we encounter a stressful situation, cortisol and DHEA are released as part of the regulation response. This is natural and good in the short-term, such as in the “fight or flight” situation. It becomes a problem, however, if the stress is chronic.
Chronic stress causes a slow down of cortisol and DHEA, potentially leading to adrenal fatigue.
When the adrenal glands are weak we no longer view stress as a challenge, but as a threat. When it’s a threat, we tend to overreact to what should be small, temporary stressors. If this frequently happens, our bodies stop differentiating between big stress (tiger) and little stress (traffic).
Ultimately the weakened adrenals set the stage for a move towards illness and disease. Left unchecked, the effects of cumulative stress can become so great that the adrenals end up completely exhausted. The end result is often feelings of deep fatigue throughout the day, unhealthy blood sugar levels, carbohydrate cravings, irritability and impaired mental functioning.
At this point the adrenals become unable to respond to any stressor, and you will see low levels of cortisol and DHEA on a blood and saliva tests.
The Domino Effect of Excess Cortisol
If the adrenal glands are healthy, they initially respond to stress by producing increased amounts of cortisol. That’s as it should be and is good in the short-term. If, however, high cortisol levels persist, metabolic and hormonal challenges will occur. High cortisol levels cause insulin resistance, and insulin resistance pushes cortisol levels even higher, resulting in a truly vicious cycle.
Insulin resistance causes weight gain, sugar cravings and constant hunger. In this state, you can also get fatigued after eating a high carbohydrate meal because the pancreas secretes more insulin than your cells can respond to.
What then happens is the body converts carbohydrates into fat, which requires energy, and which accounts for the fatigue after meals. High cortisol levels will result in symptoms of low thyroid function. When you have low thyroid function your hair may thin and some will fall out, you can become constipated, your skin may feel dry and you may feel cold most of the time. Increased cortisol also contributes to high blood pressure.
For men, chronically high cortisol levels eventually cause a drop in testosterone because cortisol blocks testosterone from working at the cell receptor sites. (Read my article on why women need testosterone.) A man will lose his sex drive and become overweight. He will frequently have high cholesterol and high triglycerides. It’s a perfect set-up for a heart attack.
In women, the brain becomes less sensitive to estrogen when there is high cortisol, resulting in hot flashes in those previously in perfect hormonal balance. Women can be surprised and confused when having “hot flashes” unassociated with menopause. The reason can be due to major stressor in their lives, which cause cortisol levels to go up, making the cells less sensitive to estrogen. Increased cortisol also occurs as a result of chronic inflammation, and chronic pain.
When cortisol is chronically elevated, the liver has a reduced ability to detoxify, promoting a leaky gut, which, in turn, can cause autoimmune reactions within the body. Increased cortisol can cause ulcers in both the stomach and small intestine, for example. Bone density can go also down.
Additionally, high cortisol levels suppress the pituitary’s ability to release luteinizing hormone, which is essential for ovulation. When cortisol suppresses ovulation it can result in infertility and diminished progesterone production. If you have too much cortisol you will also have trouble falling and staying asleep.
The reason you have a hard time sleeping is that your cortisol levels remain high at night, which is the opposite of what they should be. This can be ameliorated if you take the supplement phosphatidylserine (100-300 mg) and/or melatonin (2-5 mg) at bedtime.
Ideally, cortisol output should be at its highest when you wake up in the morning, and be at the lowest while you are asleep. Chronic stress and toxin exposure inverts this process. The result is elevated cortisol when you need to be sleeping, and that turns off melatonin and growth hormone production. Melatonin is essential for restful sleep, while growth hormone is secreted in the first two hours of sleep so that your body can regenerate itself in the first half of your sleep cycle.
De-stress Stress
I said earlier that adrenal function could be impaired by chronic stress and poor lifestyle choices. It makes sense then that you can boost your adrenal function by managing how you react to stress and by adopting a lifestyle that embraces the right foods, drinks, supplements, and if needed, pharmaceuticals.
It’s often said that stress happens “between the ears”. That’s because it’s your reaction to a potentially stressful event that creates stress, not the event itself. My favorite example is one we’ve all experienced, or certainly can relate to — a person caught in traffic.
I can remember several situations where I’d be stuck in bumper-to-bumper traffic and feeling like a fool that I’m contributing to it, and wasn’t smart enough to avoid it. I’ve learned not to get stressed in reaction to these thoughts or the event that stimulates them – the traffic — simply by observing examples of how to handle and not handle one’s reaction to traffic.
You must have seen this as well. As you’re lurching ahead during the stop and go driving spurts characteristic of traffic, inevitably you observe two dramatically different reactions to it.
The stressful reaction to traffic is the person who keeps leaning on the horn and sticks his head out of the window to shout a few invectives. The stress-less reaction is the person who is singing out loud to the groovy tunes selected on her radio, just going with the flow, even if it’s jittery and slow.
Which person are you?
The fastest way to react to stress like the gal grooving to the tunes is to be mindful of what gets you stressed out and then have a “go to place” that can relax you. When you see stress coming, practice the 4x4x4 mindfulness technique taught to the military. That’s the place you need to go.
I wrote about this mindfulness practice in Create Your Day In 5 Minutes, where I shared how “Jean” uses the method to navigate a life filled with the responsibilities of caring for her children and aging parents, which by the way is among the top instigators of chronic stress in women.
The other behavioral choices you can make to reduce stress and its impact on your adrenal glands is to get quality sleep and ingest the right foods, drinks and supplements.
Sleep
Do your best to go to bed at the same time each night (ideally no later than 11 pm), while getting at least seven to eight hours of sleep
If you anticipate that you’ll be restless while trying to sleep, try taking phosphatidylserine and/or melatonin.
Food and Drink
How often to eat and what to eat are hotly debated topics.
Many health practitioners say you should eat three main meals and two snacks every day in order to keep your blood sugar and energy stable. Others say three meals is enough and should consist of a big breakfast and lunch, and a modest dinner. On the “what to eat” topic, the debate often comes down to fats vs carbs and meat vs veggies.
Trust me, the more you dive into this stuff, the greater is the chance that you’ll get confused.
The good news is there’s some tired and true clarity when it comes to adrenal health. In this case, it’s useful not to skip meals, particularly breakfast – and to include protein with every meal, says Dr. Galzier, who makes these food and drink recommendations:
- Eat at least five to seven servings of vegetables each day, with protein.
- Never eat high glycemic foods without protein (to determine the glycemic index of the foods you eat, visit glycemicindex.com)
- Snacks are OK, but make them nuts or seeds.
- Avoid, or at least minimize, the consumption of coffee and other caffeinated products.
- Avoid alcohol, fruit juice, sugar and other sweets.
- Only use sea salt, Celtic salt, or Himalayan salt.
- Eliminate the use of all unhealthy fats, especially all trans-fats and hydrogenated oils.
Other Adrenal-beneficial Behaviors
- Stop smoking – get some help if needed.
- Try to get daily sun exposure each morning.
- Look for opportunities to laugh throughout the day.
- Meditate – here’s how.
Supplements
In addition to managing your reaction to stress via mindfulness and/or meditation and consuming the right foods, supplements can also be helpful, such as these:
(Click any of the links to see my supplement recommendations.)
| Supplement and Dose | Comment |
| Magnesium Citrate: 200 – 300 mg twice a day | 4th generation endocrinologist Dr. Thierry Hertoghe says that magnesium deficiency is the common denominator for most hormonal issues. |
| Vitamin C: 2,000 mg twice a day | Liposomal form is better absorbed. |
| B-complex vitamin once a day | Read anti-aging expert Dr. Whitaker’s advice on B vitamins here. |
| Vitamin B5: 1,000 mg once a day | |
| Vitamin E: 400 IU once a day | Select a brand that contains a full array of tocopherols and tocotrienols. |
| Vitamin D3: 5,000 IU daily | Vitamin D is actually a hormone, not a vitamin. |
| Adaptogens | Ashwaganda, Siberian ginseng, cordyceps, and Rhodiola rosea are all adaptogens and can be found as powders, tinctures or capsules. |
| Licorice | Can boost cortisol, and is also a natural antiviral agent, and can help prevent and reverse respiratory infections that often afflict persons who have adrenal fatigue. |
| DHEA: 25 to 50 mg | Like with all hormones (except perhaps vitamin D and melatonin), you should be tested for DHEA before supplementing. |
| Pregnenolone | the precursor of all the adrenal hormones… see below |
| Melatonin: 2 to 5 mg before bed. | The sublingual form is best. In addition to helping you to relax, melatonin is a potent anti-oxidant. |
| Phosphatidylserine: 100-300 mg at bedtime | |
Adrenal specialists may also give patients B complex injections and 25,000 mg of vitamin C administered intravenously once a week. Adrenal glandular extracts can also help. In cases of extreme fatigue, it may be necessary to have cortisol made by a compound pharmacy, and taken at a dose of 5mg in the morning and again at noon.
Exercise
It pains me to say this given that I pretty much believe that exercise is as close to a panacea that we’re going to find for living a long and vital life, but truth be told, if you have adrenal issues, go slow with exercise.
(Read 3 Expert-approved Anti-aging Exercise Routines.)
Any exercise that makes you feel tired, either two hours later, or the next morning, is too much for your body. Walking, slow jogging, and slow cycling are some of the best types of exercises for people with adrenal fatigue, while strenuous exercises such as circuit training, fast-paced jogging, and running on a treadmill should be avoided.
Get Your Adrenals Tested and Treated
The 60,000-dollar question is, “Are your adrenals compromised”?
There’s an pretty certain and relatively uncertain way to determine this.
Test Yourself
Testing yourself is the uncertain way to divine if you’re experiencing adrenal insufficiency. This doesn’t mean that you will not ascertain the truth, but you won’t truly know if you have or have not.
To test yourself, try to answer the following questions about yourself, but know that none are conclusive evidence that you have adrenal fatigue:
- Do you have pronated heels? Many people with adrenal fatigue do, the evidence of which can be found on the soles of their shoes, whereby the outer edge of the heels of the soles are worn down more than elsewhere.
- Are you tired all the time? Being tired after you awaken rather than being rested, or becoming tired after meals, is an indication of adrenal fatigue.
- Do you have the various symptoms of hypothyroidism or insulin resistance, either of which can be causes or exacerbated by adrenal fatigue?
- Do your pupils contract in the dark, but slowly enlarge when exposed to light? They should quickly respond to light.
- Does your systolic blood pressure number not goes up when standing? It should.
- When you lightly stroke your abdomen with the cap end of a ballpoint pen as if drawing a line, does the resulting white line return to your normal skin color within a few seconds? It should.
- Is your body temperature as measured under your armpit consistently at 98.6? This is called the “Rind Test” and it should be at or close to 98.6 degrees Fahrenheit.
If you’re interested in the specifics of doing the tests enumerated in numbers 4 through 7, read my article, Got Stress? Here Are Four Adrenal Fatigue Tests You Can Do At Home, and watch this video:
Click here for links mentioned in the video.
Get Tested
Dr. Sarah Myhill says that to know if your DHEA and cortisol is in balance, these hormones need to be measured, and the right test to do this is the
To achieve DHEA/cort balance, both hormones must be measured. This can be done with the Adrenal stress profile – salivary (ASP) test.
The Life Extension Foundation has an overwhelming number of blood, urine and salivary tests. The first one on the list is the one you want to test adrenals, the ASP. Click on the image below and check it out.
Dr. Myhill explains that the ASP test looks at cortisol and DHEA levels over 24 hours. This test entails taking salivary samples through the day (no needles!). Indeed, salivary sampling is felt to be the most accurate way of assessing steroid hormone levels.
An abnormal result may be a symptom of other problems or it may cause problems in its own right. The response of the body to stress (any stress – infectious, nutritional, emotional, physical, etc.) is to increase the output of stress hormones. This gears the body up for action by raising blood pressure, increasing heart rate, improving mental alertness (which can cause anxiety), increasing energy supply and so on.
This is metabolically inefficient because this reaction uses up a lot of energy, but totally desirable if you’re in fight or flight mode. Thus, this reaction is essential for short-term stress, but unsustainable long term.
Problems arise when the stress is unremitting. When that happens the output of the adrenal gland is reduced, making you far less able to tolerate stress.
Treatment for Adrenal Fatigue
In addition to the suggestions already made about what you can do with certain lifestyle changes, which include meditation, sleep, healthy low glycemic foods and supplements, Dr. Myhill has a treatment protocol you may consider.
She writes that she used to treat DHEA deficiency with DHEA, but now considers pregnenolone to be physiological better because it is upstream of all adrenal hormones including progesterone and cortisol.
According to Dr. Myhill, the physiological dose is pregnenolone 50 mgs. It’s better absorbed under the tongue, because sublingual doses bypass the liver – the so-called “first pass effect”.
This advice applies equally to men as it does to women. If you are taking DHEA now or if a future Adrenal Stress Profile (ASP) result shows low levels of DHEA, Dr. Myhill’s advice is that you should consider taking/swapping to pregnenolone.
For those ‘transferring’ from DHEA to pregnenolone, the conversion rate is approximately 1:2, so that if you are currently taking 25 mg daily of DHEA then you should transfer to 50 mg daily of pregnenolone, she says.
If you get to this stage, hopefully you’ll be under the supervision of an endocrinologist; perhaps this information may be vetted with him or her.
And so ends another long blog post, one I hope was useful and that you will share with everyone you think might benefit.
Last Updated on February 7, 2024 by Joe Garma