Get More Sex and A Longer Life by Supercharging Your Blood, Part 1
If living longer isn’t a good enough incentive, what about more sex? Turns out, high blood sugar and insulin desensitivity lowers your sex drive. Among other things. Here’s why…
QUICK QUESTION: What’s your fasting blood glucose number?
Most people don’t know, but there are clues.
Look down. Is your belt hidden by your gut? Are you often fatigued? Have you misplaced your libido? Do you look old?
Those are some clues that your blood sugar is too high, and with that comes a long list of unhappy results.
I’ve been busily researching material, and typing away at my soon-to-be-released (please god!) ebook, 12 Ageproof Biohacks (or some such title). Chapter 3.8 is on supercharging your blood sugar, and is about 30 pages long.
Why devote 30 pages to writing about blood sugar, also often referred to as blood glucose?
Because when your blood sugar is chronically elevated you die faster. And not just that. You also get fatter, slower, libido-less and a few other things we’ll get into in a minute.
Given all that, I was one unhappy puppy about 18 months ago when I used my sister’s blood glucose monitor to check mine.
Back then avid readers of this blog may remember me lamenting that my blood sugar (or glucose) number was so high.
I began that blog post thus:
One fine morning about a year ago, I borrowed my sister’s blood glucose meter, sat down, pricked my finger, dapped it on the strip, inserted the strip in the meter and felt my jaw bounce off the table.
This is a picture of my blood glucose result measured in milligrams per deciliter (“mg/dl”) that I measured with my ownblood glucose monitor:
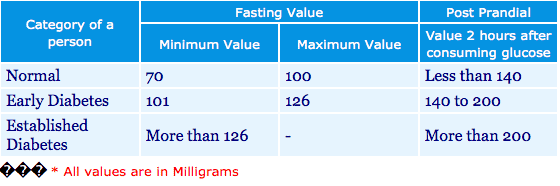
110 mg/dl fasting glucose is way too high, unless you’re fine flirting with adult-onset diabetes. According to the Life Extension Foundation:
“Prediabetes is diagnosed if the fasting blood glucose level is between 100 and 125 mg/dL. Diabetes is diagnosed if the fasting blood glucose level rises to 126 mg/dL or above.” (1)
Doctors consider any fasting blood sugar between 70 and 100 mg/dl to be normal, but several studies suggest that people whose fasting blood sugar is over 92 mg/dl are more likely to be diagnosed with diabetes over the next decade.
After I reset my jaw, I turned to my sister who was sitting next to me, and before I could blurt it out, she said, “With your diet and exercise how is this possible?”
Turns out that I’m OK, as it seems that it was the very restricted carbohydrate diet I was on that was artificially bumping up my fasting glucose numbers. (Read more about that.)
But with all the research I did on the topic, I learned that blood sugar (and insulin) is a BIG deal. You must get this right to live a long and hale life. You must get this right for your other hormones to function correctly and in balance. You must get this right to stay lean, have energy and chase your spouse around the bedroom.
The level of glucose in our blood is dependent on what kind of food is eaten and the sensitivity of insulin, a hormone produced by the pancreas to control blood glucose levels by signaling the liver, muscle and fat cells to take in glucose from the blood and use it for energy.
We “supercharge” our blood by consuming the foods and drinks that puts our blood sugar in a steady state (the focus of Part 2), thereby allowing insulin — a very important hormone — to be sensitive, or responsive to the glucose in our blood.
Our hormones are interdependent, and need to be balanced in order to properly work together to regulate physiology and behavior. When one hormone gets out of balance, it eventually disrupts the function of the others.
Sex hormones, healthy blood sugar, and insulin balance are intricately linked. Women can lose hair on their head and grow it on their face if they eat too much sugar and flour, and other high- glycemic foods that spike insulin levels sufficiently to make the body’s cells resistant to it. Men with blood glucose imbalances have trouble getting or maintaining erections, and often get “man boobs.”
These are not inevitable physiologic responses to aging. Instead, they’re the reaction to bad habits such as drinking excessive alcohol, smoking, exposure to environmental toxins, being chronically stressed, and — the grandaddy of them all — sugar, whether in the guise of corn syrup, table sugar, sugar substitutes, or fast absorbed (high-glycemic) carbohydrates, such as flour products.
Read on and learn how chronically high elevated blood sugar and the resulting insulin desensitivity can cause “diabesity”, wrinkled skin and bring you to your Maker prematurely.
Insulin Sensitivity and Diabetes
Some people are born with diabetes because their pancreas does not secrete enough insulin, a hormone that helps glucose move from the bloodstream into the cells where it’s then used for energy.
But most people with diabetes get it not by a genetically-determined malfunctioning pancreas, but by behavior. This is called “adult-onset” or “Type-2” diabetes because typically it takes years of chronically poor dietary and (no) exercise habits to slowly desensitize insulin (although these days children are getting this condition too).
Insulin-resistance occurs when the cells of our body are resistant to the glucose-lowering effects of insulin. If an individual has doesn’t produce enough insulin and/or is insulin-resistant, high blood sugar levels or diabetes will be present.
If untreated, high blood sugar levels will cause short-term effects and long-term complications.
High blood sugar levels over the short term do not cause any damage to the organs of your body; however they may cause you to feel tired and weak, be thirsty, and urinate a lot, be susceptible to infections and have blurry vision.
For the elderly, high blood sugar levels can bring on dehydration, electrolyte imbalance, and lead to falls and broken hips, a devastating injury during one’s “golden years”.
Over the long term, high blood sugar levels can cause the classic chronic complications of diabetes — eye disease (retinopathy) that leads to blindness; kidney disease or nephropathy leading to kidney failure necessitating either dialysis or transplantation; and nerve disease or neuropathy, which commonly leads to amputations. In addition, poorly controlled diabetes over the long term can also contribute to heart disease, along with inadequately controlled cholesterol and blood pressure levels.
Enough to give you pause, yes? But there’s more!
Blood Sugar and Insulin = Belly Fat
To understand the connection between blood sugar, insulin and belly fat, let’s examine a condition known as diabesity.
I don’t know if Dr. Mark Hyman coined the term “diabesity”, but certainly given the popularity of his “Blood Sugar Solution” articles, books and programs, he must be given the nod for bringing the term into the mainstream.
Dr. Hyman believes that diabesity is the number one cause of obesity, heart disease, cancer, dementia and type-2 diabetes. (2)
So, what is it?
As the name suggested, “diabesity” is a term formed from the words diabetes and obesity. What causes this potent combination are poor lifestyle choices (diet and lack of exercise) and environmental toxins interacting with one’s unique genetic proclivities.
The reason these dietary and lifestyle factors lead to diabesity is because they create insulin resistance. Type-2 diabetes is a disease of too much insulin, not too little.
Insulin is the driver of problems with diabesity, which plays out like this according to Dr. Hyman (3):
(1) A diet dominated by food and drink full of quickly-absorbed sugars (“simple” carbs) causes the pancreas to pump out increasing amounts of insulin to try to shuttle the sugar into cells for energy creation, but eventually the cells become resistant to the insulin causing more insulin to be created. The higher the insulin, the worse the insulin resistance, leading to premature aging and the diseases associated with aging, heart disease, stroke, dementia and cancer.
(2) This elevated insulin leads to the desire for more food (increased appetite), thereby increasing belly fat, causing more inflammation and oxidative stress, and a host of additional downstream effects such as high blood pressure, high cholesterol, low HDL, high triglycerides, thickening of the blood and increased risk of cancer, Alzheimer’s and depression. The source of these problems is not high blood sugar per se, but the insulting resistance (and too much insulin) that it causes.
The good news is that diabesity, and the insulin resistance that provokes it, are reversible in most cases. The body is resilient and intelligent, and will heal itself if given the chance. To help it, we must eliminate what upsets its healthy biochemistry, which will be addressed after a look at how blood sugar and insulin wrinkles our skin.
Blood Sugar and Insulin = Wrinkled Skin
Our skin is one of the most easily observable attributes of aging. It gets thin, blotchy, saggy and wrinkled. Much of this happens due to glycation, a normal process whereby the sugar in the bloodstream attaches to proteins to form harmful new molecules called advanced glycation end products (“AGEs”).
The more sugar we eat, the more AGEs both damage collagen and elastin. High sugar diets change collagen type as well.
Collagen and elastin are the protein fibers that keep skin firm and elastic. Collagen is the most prevalent protein in the body, and thus once it’s damaged, collagen and elastin’s suppleness and resilience becomes dry and brittle, leading to wrinkles and sagging.
A high-sugar diet affects what type of collagen we have. The most abundant skin collagens are types I, II, and III. Type III is the most stable and longest lasting. It’s the one we want, but glycation transforms type III collagen into the more fragile Type I, making the skin less supple.
Whats more, AGEs deactivate the body’s natural antioxidant enzymes, leaving us more vulnerable to sun damage, the main cause of premature skin aging.
That this is true is evident in those most effected by high blood sugar, diabetics, for they often have prematurely aging skin due to years of undetected high blood sugar prior to being properly diagnosed and treated.
“Depending on how well their disease is controlled, diabetics can have up to 50 times the number of AGEs in their skin as those who don’t have diabetes,” says Karyn Grossman, MD, chief of the division of dermatology at St. John’s Hospital in Santa Monica. (4)
{Read Your Battleplan To Combat Aging Skin}
Blood Sugar and Insulin Affect Lifespan
Obesity and diabetes substantially impairs healthspan (how long we live a healthy life) and longevity (how long we live irrespective of health). Both obesity and diabetes are two potential outcomes influenced by high blood and insulin desensitivity, which suggests that chronically high blood glucose itself may affect lifespan irrespective of any particular disease state that it may cause.
To understand the relationship between blood glucose and lifespan, let’s examine a 2009 study done by Dr. Anatoli Yashin and colleagues at Duke University’s Center of Population Health and Aging, which used data from 5,209 participants in the Framingham Heart Study conducted in the late 1940s, of which 993 were still alive in 2009.
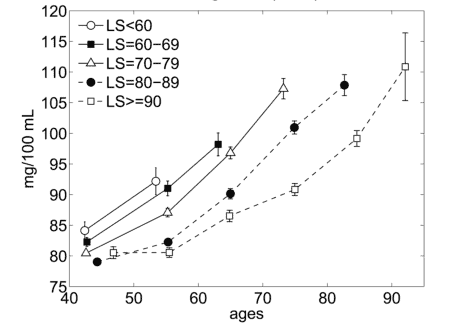
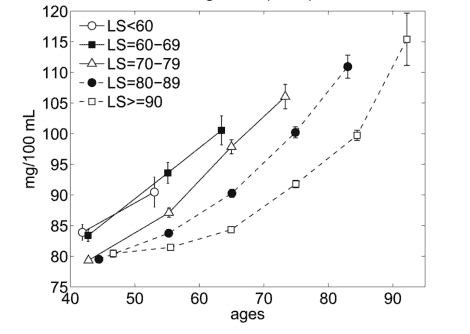
These two graphs show the studies conclusions relative to age-related blood glucose trajectories (5):
Male Blood Glucose Levels and Lifespan (“LS”)
Female Blood Glucose Levels and Lifespan (“LS”)
As you can ascertain from the figures above, blood glucose levels increase with age, even for long-lived individuals (LS > 90); however for both genders, there is an inverse relationship between glucose level and lifespan. Long-lived people have the lowest blood glucose level overall, even though it slowly increase with age in this population until approximately 55 years, whereupon it starts increasing more rapidly (steeper curve).
Assuming that their diet and lifestyle protected them, it is reasonable to argue that:
- Controlling your average blood glucose levels before you reach the age of 55 may significantly increase your chances of living beyond the age of 90;
- It’s likely that your blood glucose levels will increase with age, but slowing down that progression will increase your chances of living a longer and healthier life;
- It’s better to control reliable measures of average blood glucose levels, such as HbA1(c) and postprandial glucose levels, not fasting blood glucose levels; and
- It’s never too late to start controlling your blood glucose levels, but the longer you wait, the bigger is the risk. (6)
OK, you got all that?
Oh, hum you say… well then, let’s turn to something more savory…
Blood Sugar and Insulin Lowers Your Sex Drive (etc.)
Sugar lowers testosterone, creates leptin resistance, reduces growth hormone production, creates fatigue, and triggers anxiety and stress. World renown blood sugar expert, Dr. Mark Hyman, underscores that sugar lowers libido in five substantial ways (7):
1. Sugar lowers testosterone.
In both men and women, insulin resistance brought on by excessive amounts of sugar drives down testosterone, the hormone responsible for numerous functions including sexual well-being. The common result is that both sex drive and sexual function is impaired, as is muscle mass (decreases) and body fat (increases). Excess body fat then can increase levels of estrogen, leading to low sex drive in men and erectile dysfunction.
In a study published in Clinical Endocrinology researchers found glucose (sugar) induces a significant reduction in total and free testosterone levels in 74 men of varying ages who underwent an oral glucose tolerance test. (8)
2. Sugar creates leptin resistance.
Leptin is the hormone that signals your brain that you’re full so that you stop eating. When you eat a lot of sugar, processed foods, and flour, leptin malfunctions. Fat cells continue to produce leptin, but your brain doesn’t “pick up” the signal and eventually becomes leptin resistant. Insulin and leptin resistance often occur together.
Leptin also monitors sexual behavior. A study in the journal Clinical Endocrinology looked at three groups of men and found those with higher leptin levels had significantly higher body mass index (BMI) and lower levels of testosterone. (9)
You can see how hormones can quickly become imbalanced in a chain reaction; in this case, insulin resistance, leptin resistance, and lower testosterone.
3. Sugar reduces human growth hormone (hGH) production.
Human growth hormone (hGH) is our “fountain of youth” hormone, which is mostly produced during deep sleep. It’s secreted by the pituitary gland and substantially improves muscle mass, helps our body utilize fat, and maintain optimal libido.
Symptoms of hGH deficiencies include reduced muscle mass, increased abdominal obesity and risk for Type-2 diabetes, and lower libido.
There’s a direct link between hGH, insulin levels, and sexual function. Studies show insulin reduces our body’s ability to make growth hormone (GH), altering testosterone levels and reducing libido.
Our natural production of hGH begins to abate quite dramatically in our late twenties. Certainly, we need not spur this decline by disrupting proper insulin function.
4. Sugar makes you tired.
Sugar and other high-glycemic carbohydrates will increase blood sugar, thus requiring insulin to normalize it. Unfortunately, insulin usually over-compensates, bringing the blood sugar down too low and leading to hunger, cravings, and fatigue.
Sugar makes you tired in other ways, too. Orexin is a neurotransmitter that regulates eating behaviors, wakefulness, and arousal. The more it’s signaling, the better.
A study published in the journal Neuron found amino acids (protein) increased orexin neurons and boosted alertness, but excessive sugar did the opposite — decreased orexin, causing fatigue and drowsiness. (10)
5. Sugar triggers stress and anxiety.
Ever feel both tired and wired? Excessive amounts of sugar can do that. There’s a reason that eating five big chocolate chip cookies can make you feel full, and within an hour you get hungry again. That’s the feeling of your blood sugar crashing, leading to hunger, cravings and brain fog. Those blood sugar imbalances often trigger mood swings, depression, and anxiety — certainly not an amorous recipe.
What’s more, high insulin levels can elevate cortisol, the stress hormone. If chronically elevated, these two hormones can break down muscle mass, store fat, and dampen libido.
In Part 2 (right here), I’ll present the information and steps you need to take to supercharge your blood; meaning, what you can do to keep your blood glucose levels low and your insulin sensitivity high.
Even if you’re a processed food carb junkie with blood glucose spikes that leap over the Empire State Building, you can still heal yourself. The good news about sugar-damaged skin, belly fat caused by high blood sugar and insulin desensitivity — and even Type-2 diabetes itself — is that it’s never too late to turn back the clock.
Stay tuned.
Go to Part 2 >
P.S. Don’t miss a post, AND get on the List for the 12 Ageproof Hacks…
CONTINUE >
Would you like to learn more about Dr. Hyman’s “Blood Sugar Solution”?
 Click here!
Click here!
Further Reading:
My Blood Sugar Numbers Dumbfound Me. Part 1
Dr. Mark Hyman calls it an epidemic. Blood sugar that’s out of control is turning the people of this nation into pre-diabetics, most having no clue that they’re on the path to becoming diabetic. Is it possible, that despite all the healthy things I do, that I’m on that path too? Are you?
9 Ways to Fight Diabesity with The Blood Sugar Solution
Dr. Mark Hyman has reduced the price of this Blood Sugar Solution, a comprehensive, multi-tiered approach to fighting diabesity — the pernicious combination of diabetes and obesity that Dr. Hyman believes afflicts nearly 50% of Americans, most of whom are completely unaware. At the very least, get up to speed on this!
How Sugary Is Your Blood?
Keep The Glucose Spikes Outta Your Blood I GUESS it could be said (cause I’m about to say it) that a good diet is one that accounts for blood sugar (aka “glucose”) control. Controlling blood sugar via your diet necessitates understanding how the carbohydrates you eat effect your blood sugar. Enter the Glycemic Index (“GI”).
Sugar is a Toxin, say Three Celebrity Doctors. Watch the Interviews.
CNN’s Dr. Sanjay Gupta interviews President Clinton and sugar expert, Dr. Robert Lustig to get behind the sugar, obesity and heart disease epidemics plaguing America. Could they be related? Tips on how to reduce your sugar consumption.
Last Updated on February 25, 2024 by Joe Garma